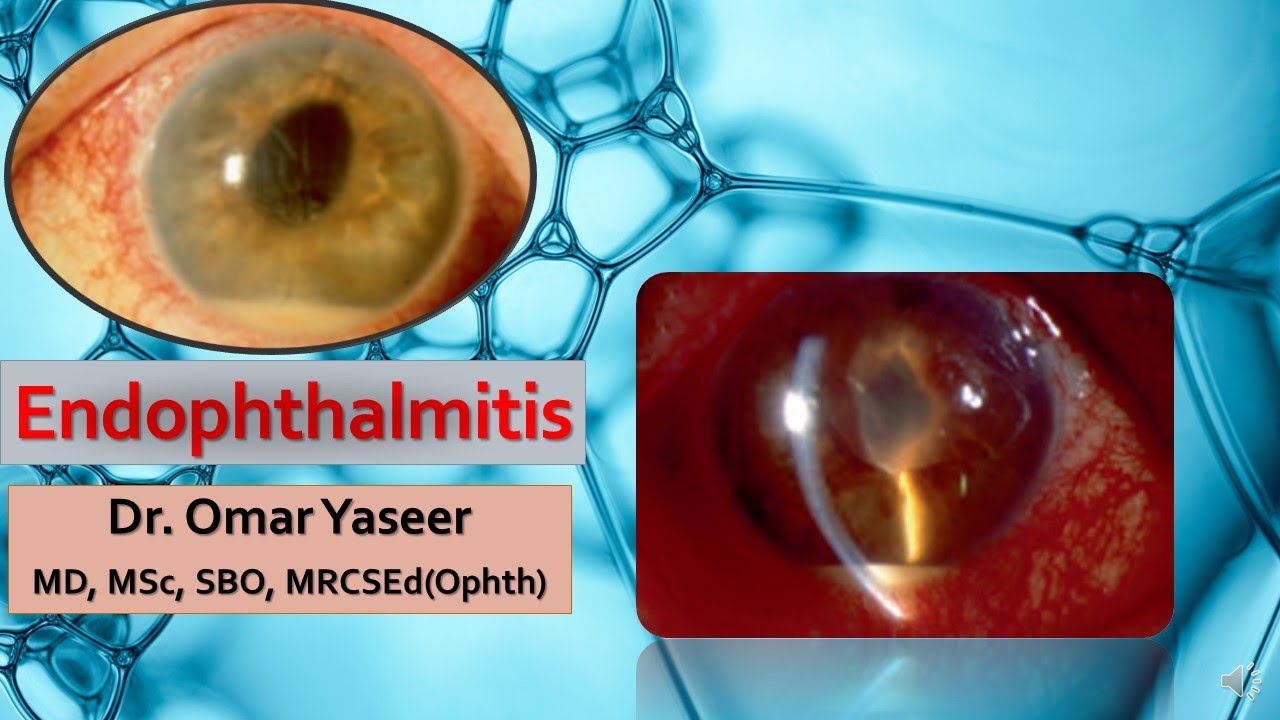
Antibiotics vs Vitrectomy for Endophthalmitis
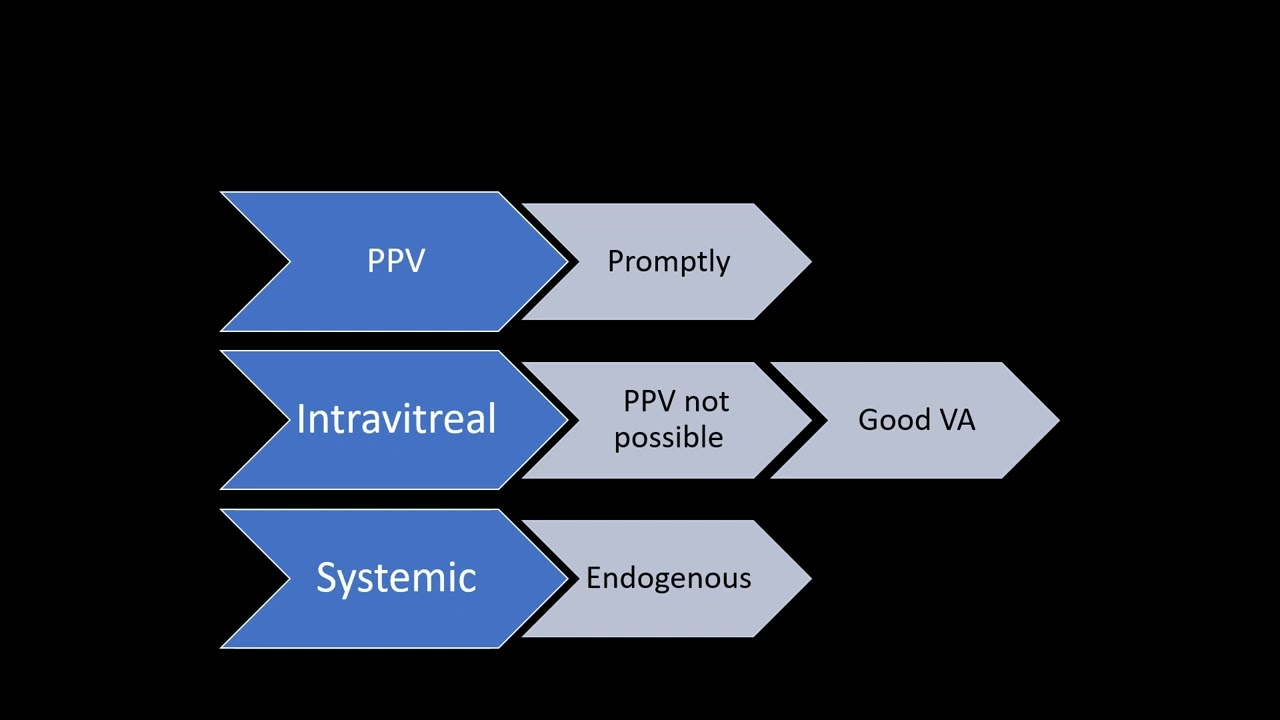
Intravitreal antibiotics vs Pars Plana Vitrectomy
Retinal Debate about the utilization of intravitreal antibiotics vs Pars Plana Vitrectomy for Endophthalmitis. In the era of vitrectomy, is there still a role for antibiotics? But if we lack facilities and experts, are antibiotics sufficient to treat this devastating disease?